Corynebacterium pseudotuberculosis is a gram-positive, intracellular, facultative anaerobic bacteria with worldwide distribution. Two biovars (variant strains) of the bacteria are present: biovar ovis is nitrate-negative and is typically found in small ruminants and cattle, causing caseous lymphadenitis, abscesses and mastitis; biovar equi is nitrate-positive and causes clinical disease in horses.
Three manifestations of the disease have been described in horses; the most common is external subcutaneous abscessation that frequently occurs in the pectoral region or ventral abdomen (hence the name ‘Pigeon Fever’). The second manifestation of the disease can cause internal abscessation, while the third manifestation causes an ulcerative lymphangitis of the limbs.
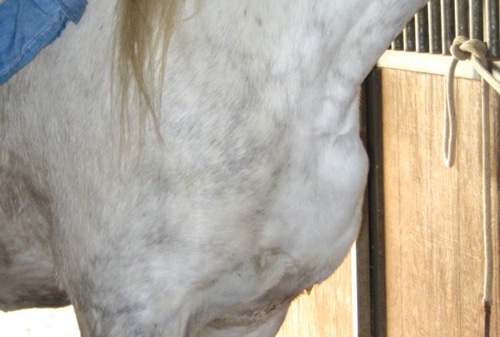
A horse with a pectoral abscess common in Pigeon Fever cases.
While internal abscessation occurs in less than 10% of C. pseudotuberculosis infections, mortality rate can range from 29% to 40% and increases to 100% among horses that do not receive antimicrobial therapy. In addition to the three classic disease manifestations, septic arthritis, osteomyelitis, guttural pouch empyema, and abortion have all been observed with C. pseudotuberculosis infection in horses.
Definitive diagnosis of C. pseudotuberculosis can be made with bacterial culture or PCR (polymerase chain reaction) test of purulent material (pus) from abscesses. Internal abscessation can be more difficult to diagnosis and often requires ultrasonography, clinicopathology and serological testing. Treatment of external abscesses may resolve with localized drainage and supportive care, while horses with internal abscesses or ulcerative lymphadenitis require prolonged systemic antimicrobial therapy.
Cause and affected regions
Infection is thought to occur through contact with contaminated soil through skin abrasions or mucous membranes. In addition, it is believed that insects such as horn flies, stable flies, and house flies act as mechanical vectors, spreading the bacteria through abrasions in the horse’s skin. Horse-to-horse transmission is also likely.
Traditionally, C. pseudotuberculosis has been associated with dry, arid climates in the western United States, with outbreaks typically occurring in the late summer or fall. However, outbreaks across the U.S. and Canada have been observed in recent years, including in non-endemic areas such as Kentucky, Louisiana, Michigan, North Carolina, South Carolina, Utah, Colorado, Oregon, Florida and Idaho. Often outbreaks are documented during dry months of the year after winters with above average rainfall, which provides optimal breeding conditions for insects during the following summer and fall. Once the bacteria become endemic in an area, infections tend to occur as sporadic cases with a prevalence of 5-10%.
Containing the disease
To limit the spread of disease, biosecurity practices should be employed, focusing on reducing environmental contamination and prevention of transmission via insects and fomites (objects likely to carry infection, such as clothing, grooming tools, buckets, etc.). Gloves should be worn while treating infected horses and all purulent material and contaminated supplies should be properly disposed of. C pseudotuberculosis is very resilient, and work by Spier et al. has shown the bacteria can survive up to eight months in soil of various moisture contents. Moreover, the addition of manure to soil enhances survival of the bacteria.
C. pseudotuberculosis was first discovered in California in 1915 and it is hard to imagine that 110 years later we would be seeing increasing cases over an increasing geographic area. Veterinarians and equine professionals cannot overlook the emotional and economic impact of this persistent disease and continued research remains warranted
The Latest












